2nd November 2021 AI provides fast, accurate diagnosis of heart failure A new algorithm created by researchers at Mount Sinai Hospital, New York, has learned to identify subtle changes in electrocardiograms (ECGs) to predict whether a patient is developing heart failure.
Heart failure, or congestive heart failure, affects about 6.2 million Americans and an estimated 40 million globally. It occurs when the heart pumps less blood than the body normally needs. For years, doctors have relied heavily on an imaging technique called an echocardiogram to assess whether a patient may be developing heart failure. This looks for irregularities in the heart using ultrasound. While helpful, echocardiograms can be labour-intensive procedures that are only offered at select hospitals. However, recent breakthroughs in artificial intelligence (AI) suggest that electrocardiograms (ECGs) – a more widely used recording device – could be a fast and readily available alternative in these cases. Electrocardiograms, as opposed to echocardiograms, use electrodes placed on the skin to detect the small electrical changes from cardiac muscle. Previous studies have shown, for example, how a deep learning algorithm working on ECG data can detect weakness in the heart's left ventricle, which pushes freshly oxygenated blood out to the rest of the body. In a new study, researchers have described an algorithm that not only assessed the strength of the left ventricle but also the right ventricle, which takes deoxygenated blood streaming in from the body and pumps it to the lungs. "We showed that deep learning algorithms can recognise blood pumping problems on both sides of the heart from ECG waveform data," said Benjamin Glicksberg, PhD, Assistant Professor of Genetics and Genomic Sciences at the Icahn School of Medicine at Mount Sinai, New York, and senior author of a study published in JACC: Cardiovascular Imaging. "Ordinarily, diagnosing these type of heart conditions requires expensive and time-consuming procedures. We hope that this algorithm will enable quicker diagnosis of heart failure."
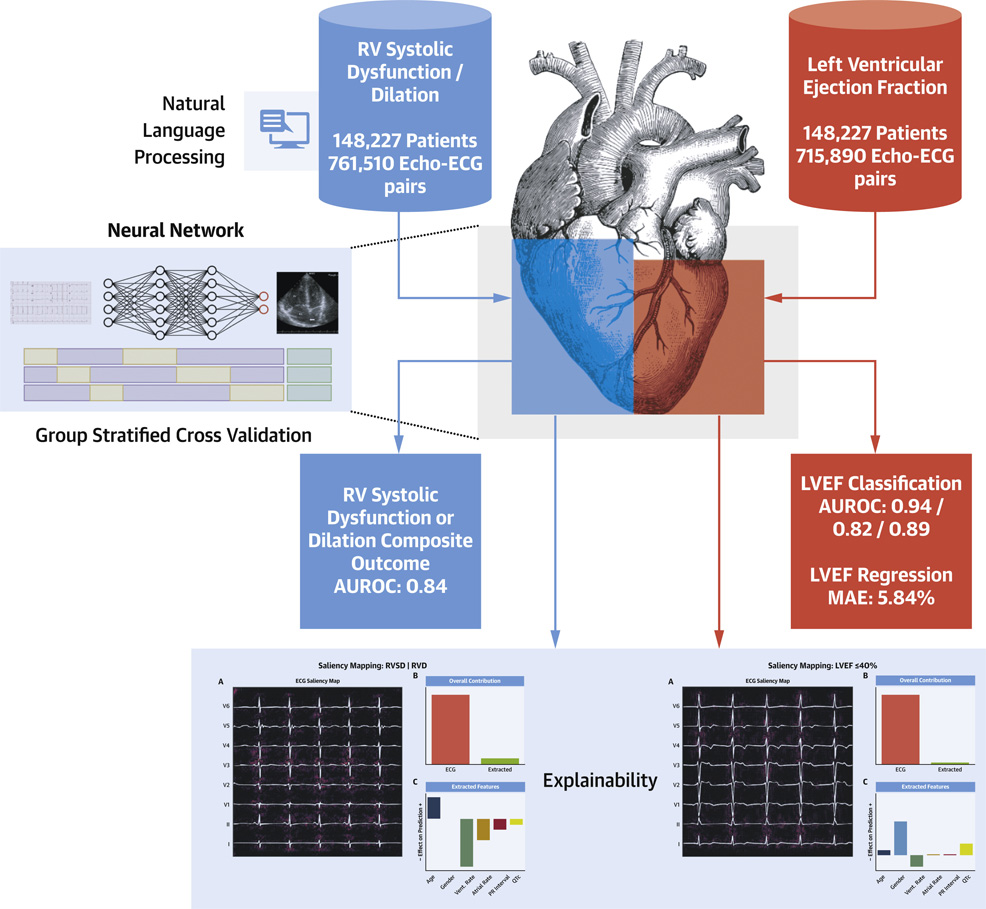
Deep-learning-based identification of left and right ventricular dysfunction from the electrocardiogram workflow. Credit: Vaid, et al. / JACC: Cardiovascular Imaging (2021)
"Although appealing, traditionally it has been challenging for physicians to use ECGs to diagnose heart failure. This is partly because there are no established diagnostic criteria for these assessments and because some changes in ECG readouts are simply too subtle for the human eye to detect," explained co-author Girish Nadkarni, Associate Professor of Medicine, who leads the Division of Data-Driven and Digital Medicine (D3M) at Mount Sinai. "This study represents an exciting step forward in finding information hidden within the ECG data, which can lead to better screening and treatment paradigms using a relatively simple and widely available test." The researchers programmed a computer to read patient electrocardiograms along with data extracted from written reports summarising the results of corresponding echocardiograms taken from the same patients. In this situation, the written reports functioned as a standard set of data for the computer to compare with the electrocardiogram data and learn how to spot weaker hearts. Natural language processing helped the computer extract data from the written reports. Meanwhile, neural networks capable of discovering patterns in images enabled the algorithm to learn and recognise heart pumping strengths. "We wanted to push the state of the art by developing AI capable of understanding the entire heart easily and inexpensively," said Dr. Akhil Vaid, who is a post-doctoral scholar in both the Glicksberg and Nadkarni labs at Mount Sinai. The computer trawled through more than 700,000 electrocardiograms and echocardiogram reports obtained from 150,000 Mount Sinai Health System patients from 2003 to 2020. This comprised data from four hospitals, with a fifth used to evaluate the algorithm in a different experimental setting. "A potential advantage of this study is that it involved one of the largest collections of ECGs from one of the most diverse patient populations in the world," said Dr. Nadkarni. The team defined healthy hearts as having a 50% or more ejection fraction – the amount of fluid a left ventricle pumps out with each beat. They defined a heart in a weak state as having a 40% or lower ejection fraction. The algorithm showed 94% accuracy in predicting which patients had a healthy ejection fraction and 87% accuracy at predicting those with weak hearts. For those patients with only a slightly weaker heart (between 40 and 50%), the algorithm had a somewhat lower accuracy of 73%. Right ventricle function proved harder to predict than left, with 84% accuracy when predicting which patients had weak right valves. The researchers trained their AI models on an NVIDIA Azure Cloud virtual machine with NVIDIA V100 Tensor Core GPUs, the world's most powerful accelerator for deep learning, which offers 32X faster throughput than a CPU. "Our results suggested that this algorithm may eventually help doctors correctly diagnose failure on either side of the heart," said Dr. Vaid. Finally, additional analysis suggested that the algorithm may be effective at detecting heart weakness in all patients, regardless of race and gender. "Our results suggest that this algorithm could be a useful tool for helping clinical practitioners combat heart failure suffered by a variety of patients," added Dr. Glicksberg. "We are in the process of carefully designing prospective trials to test out its effectiveness in a more real-world setting."
Comments »
If you enjoyed this article, please consider sharing it:
|